Young people in out-of-home care should have the same opportunities as other young people. Yet we know that these same young people have some of the poorest health and wellbeing outcomes.
While there is currently much focus on reforms in both the primary health care and the out-of-home care (OOHC) sector designed to strengthen person-centred care, particularly for people living with complex and chronic health conditions, there continues to be more to achieve to improve the outcomes for vulnerable children and young people in Victoria. Key to this is a better system response to vulnerability and complexity.
We know that the key issue for young people in residential care is their engagement with health and health services. We also know that the system response required to improve this engagement involves:
- improved service accessibility and responsiveness to specific needs of OOHC youth
- improved completion rates of OOHC health assessments
- strengthened residential staff commitment to brokering young people’s access to health services
- improved data custodianship and integration across child protection, OOHC and care teams.
SEMPHN has been working in partnership with DHHS trialling a medical home approach to address some of these barriers. The aim is for every young person in residential care to have a ‘medical home’ to provide continuity of health care. Ideally, the medical home is a multidisciplinary health clinic which is child and adolescent friendly.
The key benefits of a medical home for vulnerable young people living in residential OOHC include:
- comprehensive, whole-person care, including continuity of care, clinical integration & ehealth technologies
- relational approach to care
- shared decision-making, self-management and empowerment
- sensitivity to vulnerability and risk factors
- accessibility
- team-based care
- local healthcare pathways
- accountability, and systematic continuous quality improvement
- opportunities for patient participation in service co-design.
A systems approach for working with vulnerability
Larter supported SEMPHN in trialling the medical home approach in three sites in south eastern Melbourne. Based on this, we developed a systems approach to optimising general practice for working with vulnerability. From a primary health care perspective, a systems framework can drive a whole-of-practice approach to understanding, supporting and working through vulnerability in a way that is person-centred and ensures a safe, welcoming and inclusive healthcare environment. The following diagram depicts the building blocks which need to as a minimum underpin primary care approaches to working with vulnerable population groups, and should be used to guide next steps in building primary health care sector capacity.
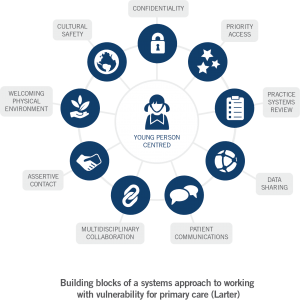
Read more in SEMPHN’s latest report on piloting the three models.
March 2018.
